Billing benchmarks
On an onboarding call earlier this year, a solo SLP in Alabama told our team: "The billing part is the part where I'm like, what have I gotten myself into." She had about a dozen clients, was doing everything herself, and said Blue Cross was just over her head. Medicaid she could figure out. But the rest of it? Too much.
We hear versions of that on nearly every onboarding call. Billing is the part that therapists dread. They went to school to help kids, not to troubleshoot payer IDs and modifier codes. So when we build billing tools at Ambiki, the question that matters most is a simple one: does it actually get better over time?
I pulled the data to find out. We looked at organizations with enough billing history to compare their first six months on the platform against their most recent six months. Five metrics, same organizations, two time periods.
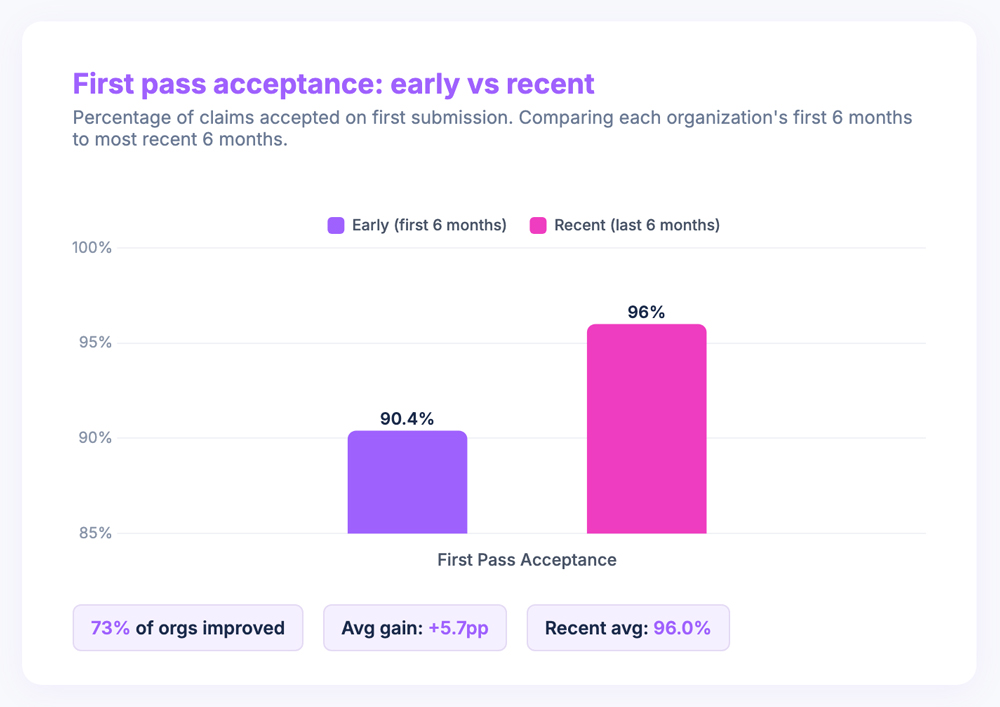
First pass acceptance was the clearest signal. 73% of organizations improved their rate, with an average gain of nearly six percentage points (from 90.4% to 96.0%). That means claims are getting accepted on the first submission more often, which means fewer resubmissions, fewer delays, fewer hours spent chasing down why something bounced. A 96% first pass rate is genuinely good. Getting there from 90% is meaningful work.
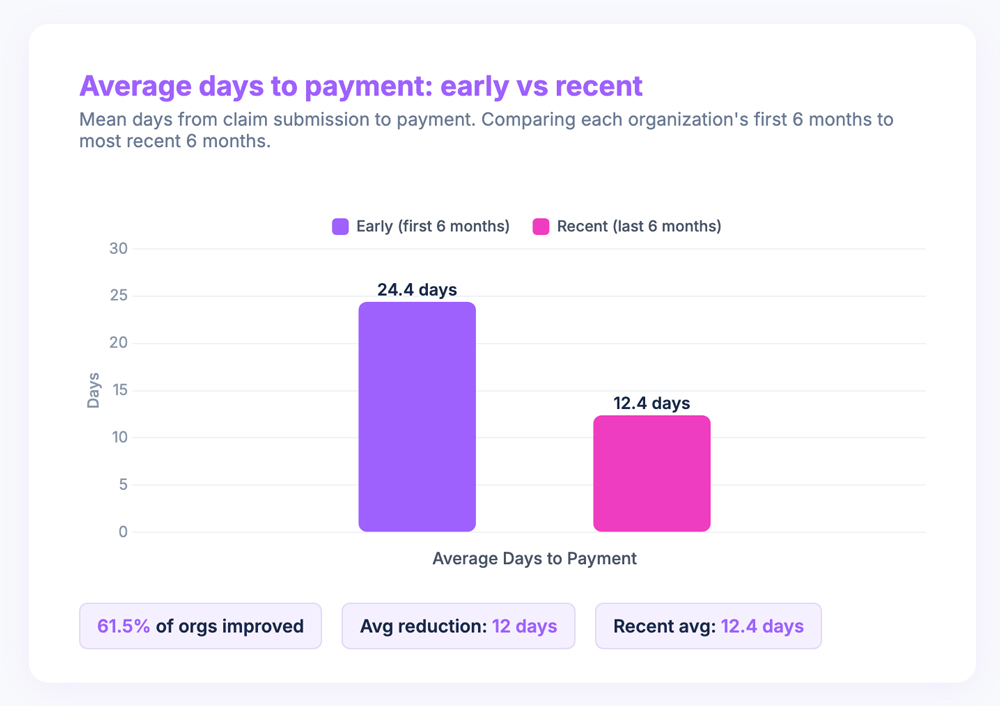
Days to payment told the next part of the story. The average dropped from 24.4 days to 12.4 days, and 61.5% of organizations improved. Getting paid in half the time changes how a small practice operates. Cash flow becomes something that just works instead of something you worry about mid-month. For a two-person clinic where the owner is also the billing manager, that shift matters.
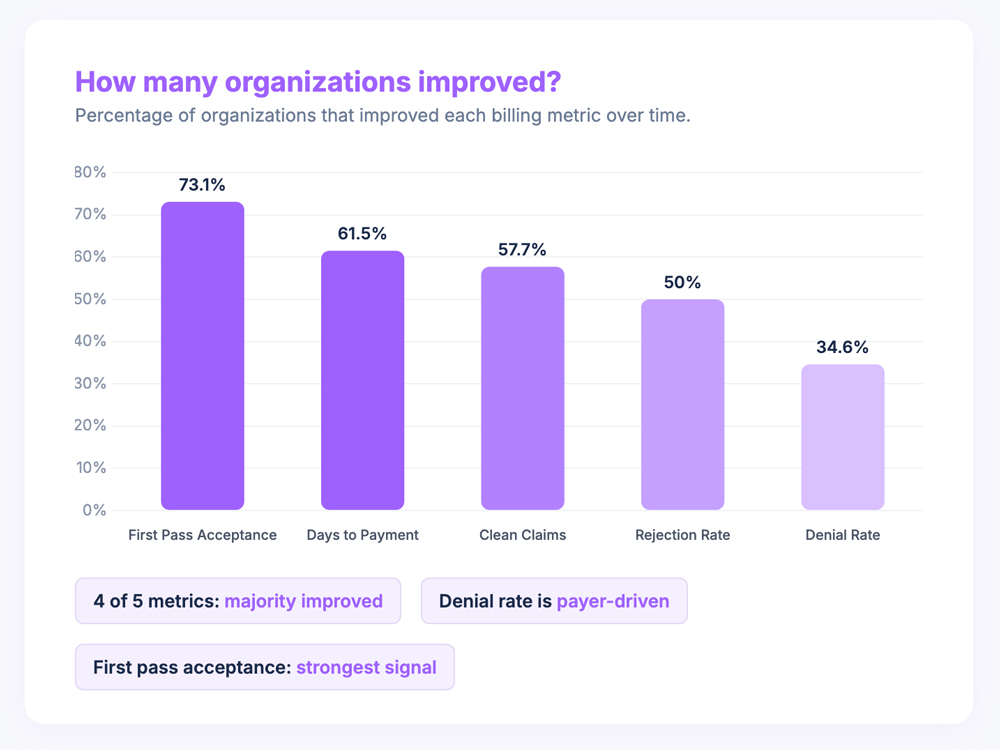
Rejection rate halved, from 2.6% to 1.3%. Half of organizations improved. Rejections are the technical errors, the wrong modifier, the missing authorization number, the mismatched NPI. They are the most preventable billing failures, and seeing them drop confirms what the first pass numbers suggest: practices are submitting cleaner claims.
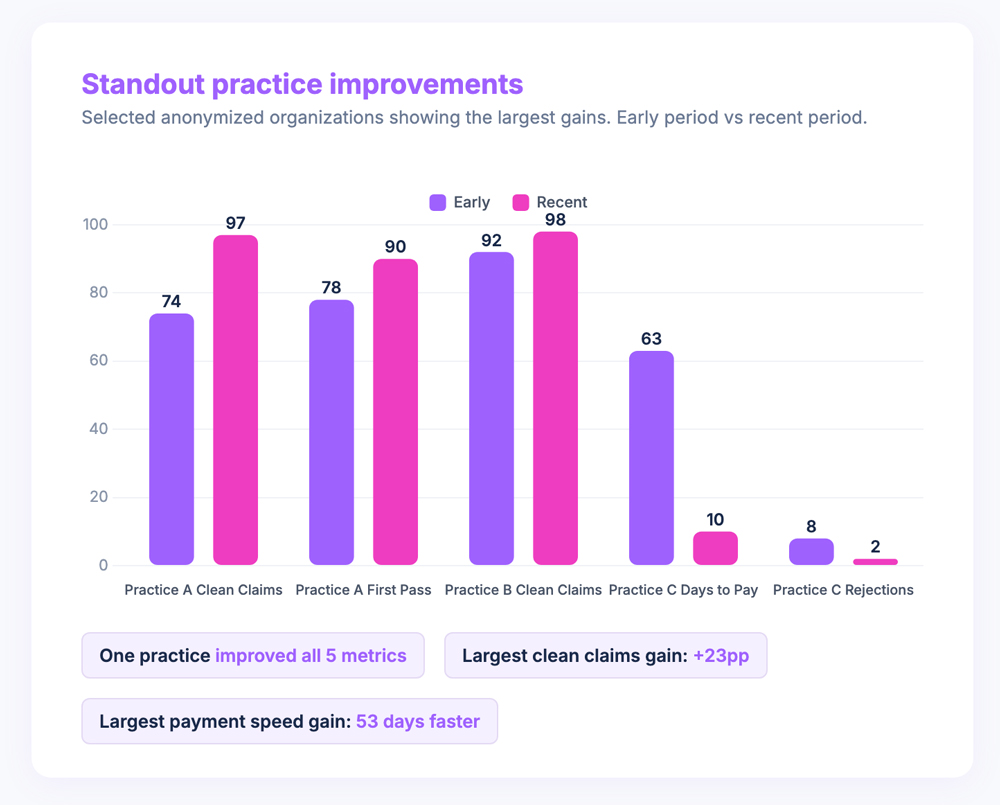
The individual stories were the most striking part of the data. One practice on Ambiki went from 74% to 97% clean claims, 78% to 90% first pass acceptance, and cut rejections from 13% to 5%. Another went from 92% to 98% clean claims while dropping denials from 8% to 1%. A third cut their average days to payment from 63 to 10, reduced denials from 15% to 9%, and brought rejections down from 8% to 2%. One practice improved across all five metrics.
These are practices that were already billing before they came to Ambiki. They had workflows, they had staff, they had payer relationships. The improvement did not come from starting at zero. It came from something shifting in how the work gets done: better claim scrubbing, faster follow-up, fewer manual errors, maybe just having the right information in front of you at the right time.
Was it the software? Was it the support and implementation teams helping practices through their first few months? The way the system guides practices toward cleaner, more consistent workflows? Probably all three, in proportions that vary by practice. The data shows that billing gets better for organizations over time after they switch to Ambiki - our team is proud of that.